Needle Exchange in San Francisco
Historical Essay
by Swetha Revanur, 2019
| Starting in the 1970s, the possession and use of drug paraphernalia was made illegal at every level of government. However, in 1988, in response to hiking HIV/AIDS rates, San Francisco volunteers at Prevention Point introduced needle exchange as a viable alternative to the criminalization of drug use. After thorough evaluations, needle exchange programs were found to be effective at reducing the spread of infections, but brought on an additional problem of safe disposal, which the city is still working through. |
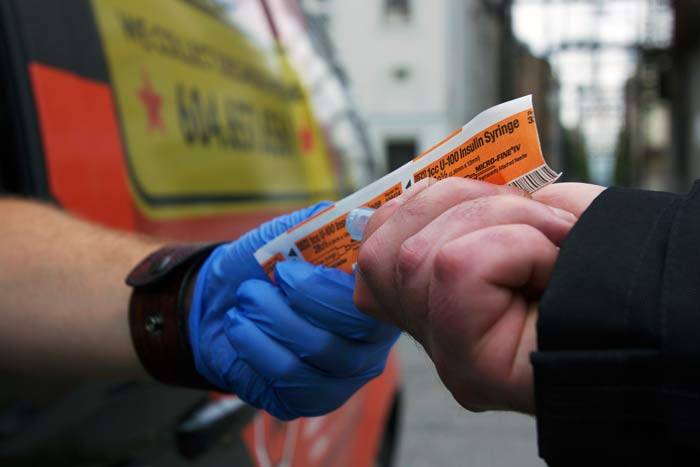
Clean syringe being distributed discreetly.
In a city that’s been hit hard by a substance abuse crisis, the number of drug addicts oftentimes surpasses the number of public high school students (Matier 2019). As of 2016, San Francisco has an estimated 22,000 intravenous drug users (Brinklow 2018) whose fix of choice is either heroin, methamphetamine, or prescription opioids. For the past few decades, San Francisco has taken major steps towards becoming a safe haven for those suffering from addiction. One of the most consequential strategies has been the needle exchange program. Needle exchanges were founded in San Francisco by people who believed that they were necessary for public health.
A Short History of Intravenous Drug Use in San Francisco
Under the Federal Drug Paraphernalia Statute of Nixon’s Controlled Substances Act, the sale and movement of drug paraphernalia, including needles, is illegal to this day (Controlled Substances Act of 1970). California state law similarly criminalized the possession of "an opium pipe or any device, contrivance, instrument, or paraphernalia used for unlawfully injecting or smoking a controlled substance" under its Health & Safety Code 11364 (Uniform Controlled Substances Act of 1972). For nearly two decades, San Francisco acquiesced to the regulations of these larger entities.
While drug use became more commonplace in the city in the 1960s—partly in response to the return of veterans who had been exposed to substances in Vietnam (Stobbe 2017)—the city’s response only took a turn when drugs began exacerbating the HIV/AIDS rates among users in the 1980s. Injection drugs contribute to HIV transmission because the virus spreads through blood and body fluids that may remain on used needles or other drug equipment. According to an annual report published by the San Francisco Department of Public Health, the number of new AIDS diagnoses was on the rise and peaked in 1992 with 212 cases among drug users (HIV/AIDS Epidemiology Annual Report 2000, p. 30).
At the time, methadone, a medication administered at special clinics, was the only addiction medication available (Vestal 2016). Although more effective than abrupt detoxification, many people stayed on methadone maintenance for years, leading to the “continued provision of an addicting drug” (Harris 2000). The limited options led to escalating anguish within the HIV-positive addiction-riddled community that engendered furor on the streets.
The Humble Beginnings of Needle Exchange
Born out of an act of self-determination and protest, a group of San Francisco volunteers established Prevention Point, the city’s first needle exchange program, in 1988 (San Francisco AIDS Foundation). Though in explicit defiance of municipal, state, and federal laws, Prevention Point’s strategy altered both the course of the AIDS epidemic and the relationship between city authorities and drug users. Their program offered safe injection equipment, condoms, and social services to those on the streets. “For nearly four years, Prevention Point operated totally underground. Volunteers actually used a baby carriage to transport sterile syringes to neighborhoods that needed them most.” They painstakingly documented trends in the relationship between syringe access and HIV.
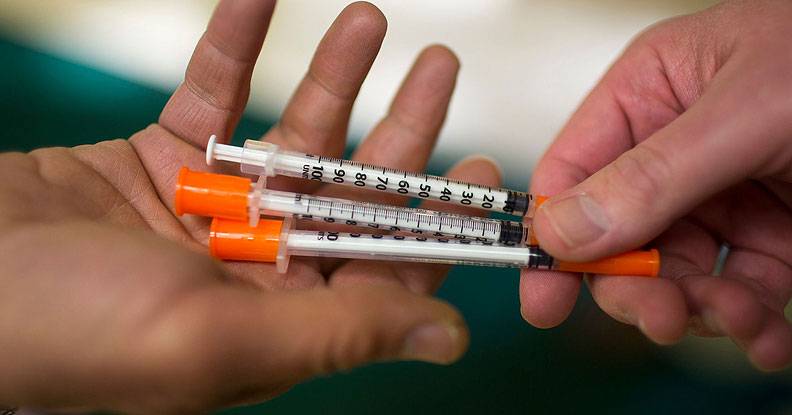
Needle exchange.
Photo: HuffPost
In March of 1993, the Los Angeles Times published an article announcing San Francisco Mayor Frank Jordan’s pledge to “give clean needles to drug users in a campaign to halt the spread of AIDS” (Paddock 1993). Jordan promised $138,000 to support Prevention Point’s efforts, catalyzing San Francisco’s move away from a war on drugs. Needle distribution and exchange immediately became the linchpin in its synchronous move towards harm reduction services. “When the program began, people were provided with 10 syringes with a one-for-one exchange above the 10 returned. In 1990, participants were allowed to access 20 syringes at one time instead of 10. In August of 1990, all limits on the number of syringes that could be accessed were lifted” (San Francisco AIDS Foundation).
The social movement that sprung out of needle exchanges was a cross-cultural one. Glide Memorial Church, a leading organization in the civil rights movement, quickly rose up to be one of San Francisco’s primary needle exchange providers in the Tenderloin. The Tenderloin is a neighborhood in downtown San Francisco with the city’s highest rates of homelessness and intravenous drug use. Glide staffers walk through the streets, religiously distributing needles, safe disposal bins, and naloxone refills, only a few blocks from “the shiny offices of Twitter, Square, and Uber” (Lurie 2017).
The Efficacy of Needle Exchange
The reason so many San Francisco institutions bought into the idea of needle exchange was because of its efficacy. It is one of the most widely debated topics when it comes to American healthcare, and as a result, “it is the most thoroughly studied public health intervention of the past thirty years” (Homeless Youth Alliance). In 2012, Tookes et al. from the University of Miami published a comparative study between San Francisco and Miami, a city without needle exchanges. There was an eightfold difference in the number of syringes found on the streets in Miami, and “[injection drug users] in Miami had over 34 times the [odds] of public syringe disposal relative to [injection drug users] in San Francisco.” Other studies have had similar findings, with one from Takács et al. stating that “the providing of needle and syringe programs are an indispensable condition of successfully preventing the spread of HIV.”
In their book, Righteous Dopefiend, Jeff Schonberg and Philippe Bourgois tell the stories of homeless residents in San Francisco’s Mission District. When needle exchange activists began more strongly regulating syringe access, residents “stopped regularly visiting the needle exchanges that formerly had been their primary source of clean needles” (Schonberg and Bourgois 2009, p. 222). More than providing syringes, these programs had become the sole path to treatment and medical services for their clients. Across the city, the existence of needle exchanges has become an unambiguous and critical determinant of health in their operational areas.
Critical Perspectives
Nevertheless, critics of needle exchange point to disposal as their primary concern. They claim that controlling safe access to needles requires that the city also controls safe disposal. Unfortunately, recollection is not San Francisco’s strong suit, and needle exchanges don’t actually require that dirty syringes be returned. An article in the San Francisco Chronicle found that the city collects only 60 percent of all distributed syringes (Brinklow 2018). Over the years, investigative reports surveying dozens of city blocks liken San Francisco to the world’s most impoverished slums (Shaban 2018), in part due to the ubiquity of needles in public places. Needlestick injuries can transmit blood-borne viruses, and are a grave concern around children’s play areas.
In the 2016-17 fiscal year, San Francisco spent $35 million on street cleaning alone, leagues more than comparable cities (Matier & Ross 2018). Advocates—including Mayor London Breed (Zezima 2019)—are offering an alternative: safe injection sites. Safe injection sites are hygienic medical facilities where users can inject intravenous drugs under supervision and subsequently dispose of their drug paraphernalia. As of 2019, there are no consumption rooms in the United States because their efficacy is still being evaluated.
Needle exchange supplies.
Conclusion
Although not a perfect solution, many San Franciscans have found refuge in needle exchanges. A Harm Reduction Coalition client wrote, “I first injected in high school. It was a small miracle I didn’t get infected with HIV or hepatitis at that time, since I had no idea where to get sterile syringes…” Since discovering a local needle exchange, the person has been clean for 7 years without HIV or hepatitis, and holds a graduate degree in public health (Harm Reduction Coalition). It is success stories like that one that continue to drive the search for an intervention that both reduces drug use and offers a support system for those still struggling.
Works Cited
Brinklow, A. (2018). City Hall hands out 4.45 million syringes each year, says report. CurbedSF.
Controlled Substances Act. 21 U.S. Code § 812. (1970).
Harm Reduction Coalition. Personal Testimonies.
Harris, L. (2000). Methadone maintenance found to be more effective in treating heroin addiction than 180 day detoxification. UCSF News.
Homeless Youth Alliance. Needle Exchange FAQ.
Lurie, J. (2017). “I Love My Job”: Fighting Addiction and Overdoses on the Streets of San Francisco. Mother Jones.
Matier, P. (2019). San Francisco — where drug addicts outnumber high school students. San Francisco Chronicle.
Matier, P., & Ross A. (2018). SF’s filthy streets: We’re spending far more on cleaning than other cities. San Francisco Chronicle.
Paddock, R. (1993). S.F. Will Provide Drug Users With Clean Needles : Health: The mayor, citing the spread of AIDS, declares a citywide emergency to skirt state law prohibiting distribution of hypodermics. Los Angeles Times.
San Francisco AIDS Foundation. History of Health: Needle Exchange in San Francisco.
San Francisco Department of Public Health. (2000). HIV/AIDS Epidemiology Annual Report. pdf
Schonberg, J., & Bourgois, P. (2009). Righteous Dopefiend.
Shaban, B. et al. (2018). Diseased Streets. NBC Bay Area.
Stobbe, M. (2017). Today's opioid crisis shares chilling similarities with past drug epidemics. Chicago Tribune.
Takács, I. (2009). The efficacy of needle exchange programs in the prevention of HIV and hepatitis infection among injecting drug users. Psychiatria Hungarica.
Tookes, H. et al. (2010). A comparison of syringe disposal practices among injection drug users in a city with versus a city without needle and syringe programs. Drug and Alcohol Dependence.
Uniform Controlled Substances Act. California Health and Safety Code (1972).
Vestal, C. (2016). Few Doctors Are Willing, Able To Prescribe Powerful Anti-Addiction Drugs. Pew Stateline.
Zezima, K. (2019). California Assembly approves supervised opioid injection facility, faces federal opposition. The Washington Post.